Stevens-Johnson syndrome and toxic epidermal necrolysis: Difference between revisions
(→Source) |
No edit summary |
||
| Line 10: | Line 10: | ||
**Infectious | **Infectious | ||
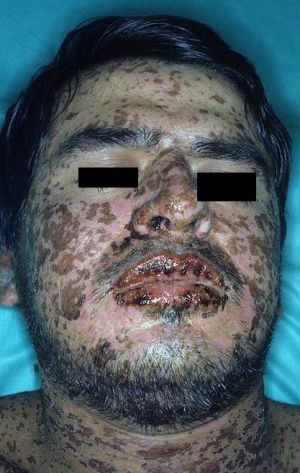
[[File:Stevens-johnson-syndrome.jpg|thumbnail|Stevens–Johnson syndrome]] | [[File:Stevens-johnson-syndrome.jpg|thumbnail|Stevens–Johnson syndrome]] | ||
[[File:SJS.jpg|thumbnail|Mucosal lesions with Stevens-Johnson]] | [[File:SJS.jpg|thumbnail|Mucosal lesions with Stevens-Johnson]] | ||
==Clinical Features== | |||
*Often have prodrome (fever, URI symptoms, HA, malaise) | *Often have prodrome (fever, URI symptoms, HA, malaise) | ||
*Macular rash | *Macular rash | ||
| Line 22: | Line 23: | ||
**Eye involvement can be severe | **Eye involvement can be severe | ||
*In severe cases, respiratory tract and GI involvement may occur | *In severe cases, respiratory tract and GI involvement may occur | ||
==Differential Diagnosis== | ==Differential Diagnosis== | ||
| Line 37: | Line 31: | ||
*[[Drug eruption]] | *[[Drug eruption]] | ||
== | ==Diagnosis== | ||
===Work-Up=== | |||
*CBC | |||
*CMP | |||
*ESR | |||
*CXR | |||
*Examine eyes/mucosal surfaces | |||
===Evaluation=== | |||
*Clinical diagnosis | |||
==Management== | |||
*Removal of inciting cause if identified | *Removal of inciting cause if identified | ||
*Fluid replacement - treat shock w/ IV fluids according to burn protocols | *Fluid replacement - treat shock w/ IV fluids according to burn protocols | ||
| Line 44: | Line 49: | ||
*Use of IVIG, plasmapheresis, and corticosteroids are controversial but may be beneficial | *Use of IVIG, plasmapheresis, and corticosteroids are controversial but may be beneficial | ||
== | ===Prognosis=== | ||
== | |||
Validated with SCORTEN mortality assessment: | Validated with SCORTEN mortality assessment: | ||
| Line 72: | Line 74: | ||
5+ (90.0%) | 5+ (90.0%) | ||
== | ==Disposition== | ||
* | *Admit to burn unit or ICU | ||
==See Also== | ==See Also== | ||
*[[Rashes]] | *[[Rashes]] | ||
==References== | |||
<References/> | |||
[[Category:Derm]] | [[Category:Derm]] | ||
[[Category:Drugs]] | |||
[[Category:Critical Care]] | |||
Revision as of 11:15, 17 August 2015
Background
- SJS and TEN exist on a spectrum of disease
- SJS involves <10% of BSA
- TEN involves >30% of BSA
- Dermatologic emergency
- Causes:
- Drugs - many. Common offensive agents include: quinolones, sulfa, PCN, ASA, acetaminophen, carbamazepine, NSAIDs, phenytoin, corticosteroids, immunizations
- Malignancy - lymphoma
- Idiopathic
- Infectious
Clinical Features
- Often have prodrome (fever, URI symptoms, HA, malaise)
- Macular rash
- +/- Target lesions
- Usually starts centrally, spreads peripherally, and may become confluent
- May be painful
- May have +Nikolsky sign (denude when touched)
- Mucous membranes can be severely affected
- Eye involvement can be severe
- In severe cases, respiratory tract and GI involvement may occur
Differential Diagnosis
- Erythema Multiforme
- Staphlococcal scalded skin syndrome
- Erythroderma
- Toxic Shock Syndrome
- Drug eruption
Diagnosis
Work-Up
- CBC
- CMP
- ESR
- CXR
- Examine eyes/mucosal surfaces
Evaluation
- Clinical diagnosis
Management
- Removal of inciting cause if identified
- Fluid replacement - treat shock w/ IV fluids according to burn protocols
- Infection control
- Wound care
- Use of IVIG, plasmapheresis, and corticosteroids are controversial but may be beneficial
Prognosis
Validated with SCORTEN mortality assessment:
One point for each of the following assessed within 1st 24 hours of admission:
- Age >/= 40 years (OR 2.7)
- Heart Rate >/= 120 beats per minute (OR 2.7)
- Cancer/Hematologic malignancy (OR 4.4)
- Body surface area on day 1 >10% (OR2.9)
- Serum urea level (BUN) >28mg/dL (>10mmol/L) (OR 2.5)
- Serum bicarbonate <20mmol/L (OR 4.3)
- Serum glucose > 252mg/dL (>14mmol/L) (OR5.3)
Predicted mortality based on above total:
Score 0-1 (3.2%)
2 (12.1%)
3 (35.3%)
4 (58.3%)
5+ (90.0%)
Disposition
- Admit to burn unit or ICU